[Local Medical]Vaccine Screening Treatment 3 Strategies to Eliminate Cervical Cancer
[ad_1]
Text Yang Qianni Organized Liang Yingxiu
The elimination of cervical cancer mainly relies on the three strategies of vaccine, screening and treatment.
Cervical cancer is mainly caused by human papillomavirus (HPV), more specifically high-risk strains such as HPV16 and HPV18.
Dr. Dato’ Abdul Aziyah
(Dato Dr Abd Aziz Yahya)
(KUALA LUMPUR): Since 2018, the World Health Organization (WHO) has formulated a strategic plan to try to eliminate cervical cancer. It was a very brave decision — rather than continue to screen to prevent it, try to prevent it from happening.
Improving HPV Vaccination Rates First
Based on the discovery of the main cause of cervical cancer by the medical community and the development of vaccines, Dr. Dato Dr Abd Aziz Yahya, a consultant obstetrician and gynecologist, believes that it is possible to eliminate this cancer.
“In November 2020, WHO announced that the world will commit to eliminating cervical cancer, defined as the annual incidence rate falling below 4 per 100,000 population. Although it seems difficult to achieve, I believe that as long as continuous efforts can be successful , especially in a smaller country like Malaysia. In order to move towards this goal, WHO has proposed three major strategies, namely vaccines, screening and treatment.”
“The first is to increase HPV vaccination coverage, we need to get 90% of women vaccinated against HPV by the age of 15.
There are currently 111 countries with HPV vaccination programs for girls under 15, which is pretty good, but it could be better. To achieve the elimination goal, every country in the world should follow the plan proposed by WHO. “
At present, our country is implementing a free HPV vaccination program for 13-year-old female students in schools. If they miss the vaccination, try to get them done before the age of 15. However, vaccinations are limited to girls only.
He said that there are 40 countries in the world where the HPV vaccine is also administered to men, and he also has his son vaccinated against HPV. If you understand the pathology of cervical cancer, you will find that men can transmit the HPV virus to women, which allows them to protect themselves and their partners.
Therefore, it would be better if the HPV vaccine could be vaccinated for both sexes.
“Australia was the first to include the HPV vaccine in its national free vaccination program in 2007 and included boys in 2013. Most countries that have introduced HPV immunization programs are known to have successfully reduced the incidence of cervical cancer and precancerous lesions .
Sixty percent of new cases now occur in countries that do not offer HPV vaccination on a large scale, such as China and India. Therefore, achieving the goal of eliminating cervical cancer will be difficult unless these two large countries can also provide HPV vaccination to their populations. “
He said that if memory serves me correctly, about two or three years after the first HPV quadrivalent vaccine came out in 2006, Malaysia included it in the national immunization plan. At present, the bivalent vaccine is mainly used in the national immunization program of Malaysia. “The quadrivalent vaccine has also been improved to nine valent, which can prevent nine types of cancer-causing HPV viruses, but its cost is much higher.”
Incomplete cervical cancer screening program
In addition, the HPV vaccine is expected to provide lifelong protection for the vaccinated, so it can be vaccinated even in the 40s and 50s. The medical community is still following up the first batch of women who received the HPV vaccine in 2000 and found that there is still enough protection so far, so the vaccinators should not need to receive booster shots.
The second major strategy proposed by WHO is to increase the screening rate and accuracy. 70% of women must have received accurate screening at least twice before the age of 35 and 45.
“Most people know that pap smear (pap smear), or cervical cytology (cervical cytology), has two methods, that is, traditional smear test and liquid-based cytology test. Two The latter obtains cervical cells in the same way, except that the latter does not smear the cells on a glass slide, but puts them in a special preservation solution, and then uses an instrument to make an ultra-thin smear for interpretation, with higher accuracy.”
While Pap smears are repeated year after year, we do realize that it does not reduce the incidence of cervical cancer, let alone achieve its elimination.
“Of course, the increase in the incidence rate is caused by multiple factors. One is that the vaccination coverage rate is not high enough, and the other is that there are not enough Pap smears.”
He pointed out that our country also lacks a relatively complete cervical cancer screening program. Usually, women “come when they want to”, and sometimes doctors do not do enough to allow sexually active women to undergo regular Pap smears.
“While we have some medical services available, they are not accessible to all women. So, there should be some barriers in between, maybe try less cumbersome and more accurate screening? That’s what we discussed. The reason for HPV screening every 5 years.”
Since most cervical cancers are caused by oncogenic strains of HPV, why not check for that virus specifically?
“In addition to the less frequent frequency, women can also take samples and send them for testing. If some women can’t come to the hospital, they can also be taught how to take samples through videos or templates. In this way, it is expected to increase women’s chances of being screened.”
Screening once reduces the risk of death by 87%
The 2014 Australian clinical trial COMPASS found that self-sampling HPV screening restrictions reduced the incidence of cervical cancer and increased the detection rate (pickup rate).
“When abnormalities are found in the screening, patients can receive treatment earlier without waiting for a cancer diagnosis. Australia has switched from traditional cytology to HPV screening, coupled with its implementation of ‘both men and women’ HPV immunization I believe Australia will be the first country in the world to eliminate cervical cancer in the next 10 years.”
He emphasized that, regardless of whether it is a cervical smear or HPV genotyping test, a woman who receives only one screening can reduce the risk of death by 87%, because most cases can be found at the stage of precancerous lesions. “Therefore, we should continue to encourage women to be screened regularly, and it may be medically appropriate to consider changing the way screening is done in our country.”
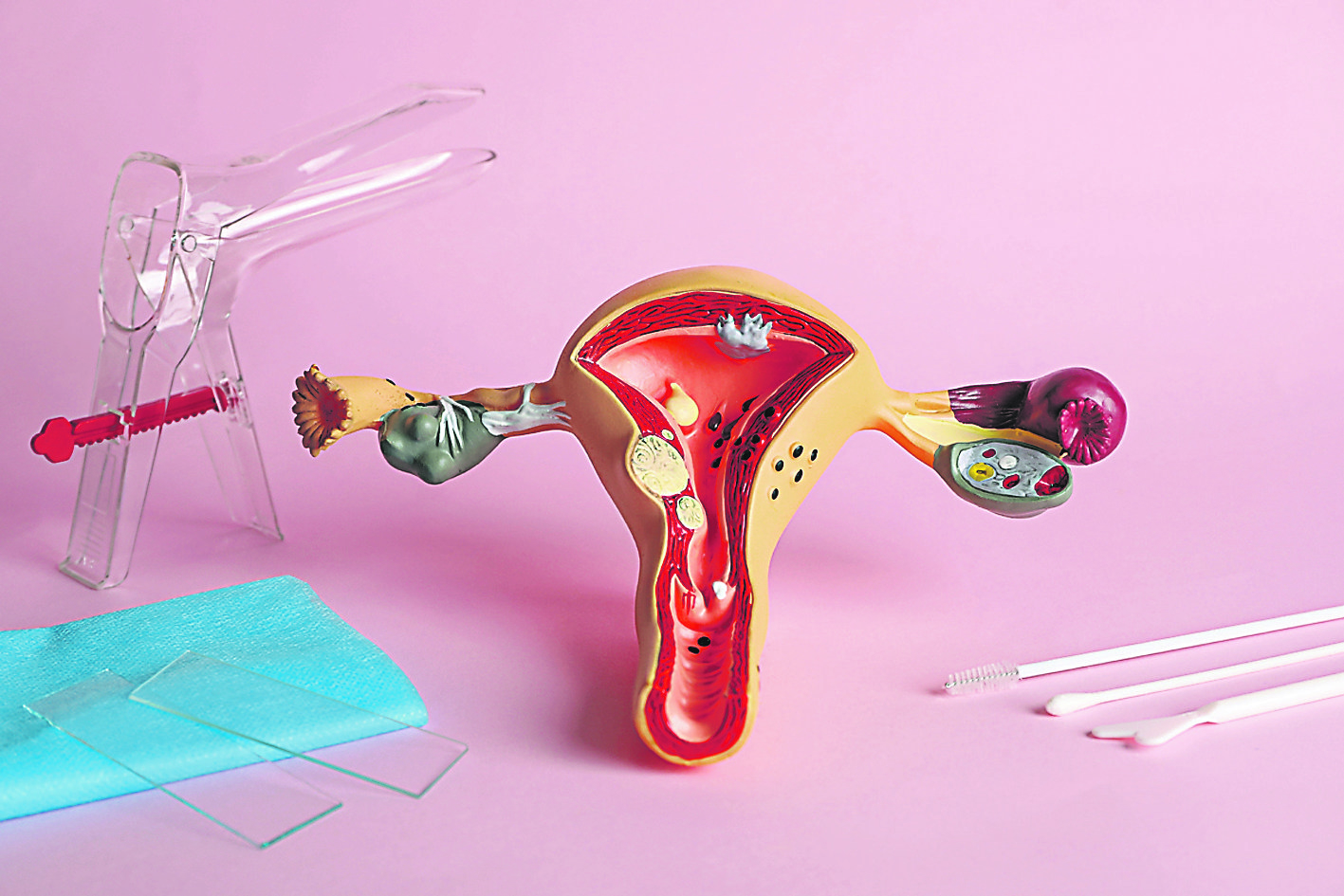

Get screened and know the result
The third major strategy to eliminate cervical cancer is to allow 90% of diagnosed patients to receive due treatment.
People in different countries also have different restrictions on access to medical services, such as formal surgery, chemotherapy or radiotherapy.
The level of medical care in Malaysia is not bad, because it can provide patients with a full range of treatment methods.
Abdul Aziyah pointed out that after undergoing the screening, one must know the result. Unfortunately, often when he asked cancer patients, most patients always said that they had undergone examinations several years ago, but they did not know whether the results were normal or not.
Cervical cancer undergoes precancerous lesions
“For the hospital, who is responsible for contacting the patient after the interpretation report is abnormal? This shows that the hospital’s call and recall (call and recall) system is very important.”
“When the screening test is normal, then the woman can repeat the Pap smear after 1 or 2 years; if the result is abnormal, she should be referred to the obstetrics and gynecology department for colposcopy. Colposcopy is a similar The instrument of the magnifying glass can magnify the image 50 times, which is helpful to observe the subtle lesions of the cervix.”
“Cervical cancer doesn’t develop overnight,
They first undergo a precancerous lesion called cervical intraepithelial neoplasia
(Cervical Intraepithelial Neoplasia, CIN) to stages I to III.
It usually takes 10 years to develop from CIN 1 to 3,
It takes about 5 years for CIN 3 to develop into cancer.
Therefore, women have about 10 to 15 years to detect abnormalities,
Get treatment to avoid cervical cancer. “
He pointed out that colposcopy can choose local or general anesthesia. If a lesion is found, the doctor will perform a cone biopsy. The patient will keep the uterus and ovaries, etc., and only suspicious tissues showing CIN will be removed. The grade of CIN can be determined at the follow-up visit one week later. Treatment ends after complete resection, and screening can be repeated at a later date.
“Thus, treatment during this period is conservative, inexpensive, low-risk, and does not result in loss of fertility.”
Chemotherapy after lymphatic involvement
The treatment for cervical cancer is surgery, chemotherapy or radiotherapy. “Stage I and II cervical cancers can undergo radical hysterectomy (Wertheim). It is a major surgery that takes about 3 hours and has some risks. Patients may require intensive care unit (ICU) care after surgery. More advanced cervical cancer is usually performed pelvic exenteration (pelvic exenteration).
“Missing the opportunity to detect precancerous lesions will change the patient from a simple colposcopy and tissue removal treatment to a major operation requiring removal of the uterus, cervix, ovaries and lymph nodes, with risks, side effects, complications and mortality. It has also improved. If the lymph nodes are involved, the patient will need chemotherapy or radiotherapy after surgery, which shows that the cost will be greatly increased. In this case, why did we go to this point?”
[ad_2]
Source link

![[Love Wants Sexual Happiness Series 358]Find the culprit and overcome psychogenic erectile dysfunction. Don’t let pressure affect your sexual happiness.](https://chinathenews.com/wp-content/uploads/2024/04/171111-780x420.jpg)

![[Wanqingyi Care]My health, my rights, customized medical methods in the last stage of life](https://chinathenews.com/wp-content/uploads/2024/04/ZZ1-100-780x420.jpg)
![[Kidney Transplantation Special Topic]The survival rate of transplanted kidneys is high without dialysis treatment three times a week](https://chinathenews.com/wp-content/uploads/2024/04/1311-780x420.jpg)



